These are very unprecedented times. We are no longer dealing with the same challenges as we were before. Times where we knew how not to spread HIV/AIDS or at least contain it. We could easily treat or prevent Sexually Transmitted Infections and disease (STDs/STIs). And now? Chlamydia, Gonorrhoea, Syphilis and even THE HIV/AIDs itself are no match for the Novel Corona virus.
These are indeed very uncertain times, with governments all over the world taking drastic measures to lock down, restrict movements and yet with diminutive hope or certainty that things will go back to normal soon.
Take caution :
With most people working from home or on forced leave and movement restrictions, loneliness, boredom with the so much time is paramount. For those staying with their partners the idea of sex must be flaunting. I mean ‘things’ are freely available on full time basis right?
Please note: Even if you are under self or institutional quarantine, having unprotected sex will still expose you to STIs and STDs and unplanned pregnancies.
But since abstinence is a complicated subject even without the CORONA virus, how can one enjoy their things without fear of getting pregnant or contracting STDS or STIs?
How do i not get pregnant?
Using contraceptives allows people to attain their desired number of children and determine the spacing of pregnancies. They are also very helpful in times such as these where one wouldn’t want to get pregnant.
There are however two methods one can use to delay pregnancy; Traditional and modern methods these are broken down below;
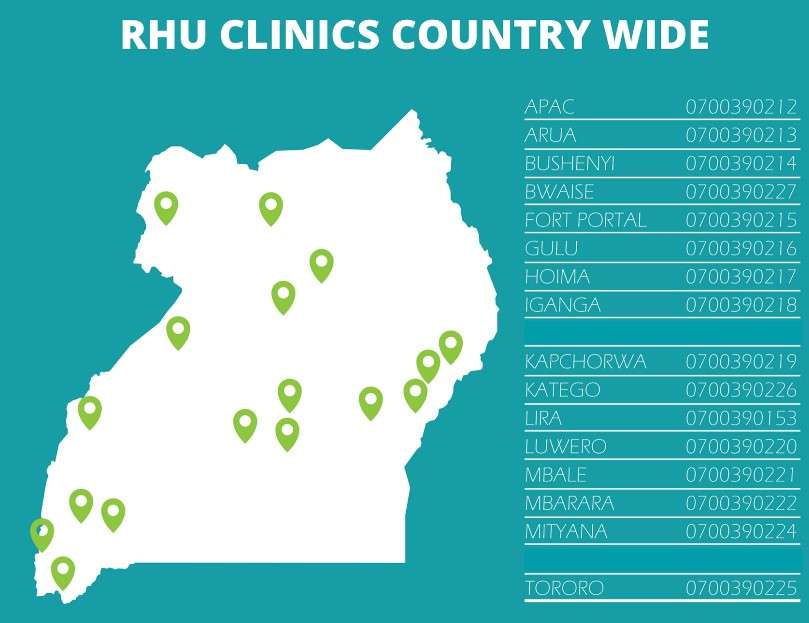
Reproductive Health Uganda clinics remain open across the country You can call any of the clinics in charges for appointments and or questions
What are the Modern methods?
PS: We recommend using modern methods because of their accuracy. They can easily be relied on without fear. These methods are available at any of the Reproductive Health Clinics countrywide. Give us a call to make an appointment
| Method | Description | How it works | Effectiveness to prevent pregnancy | Comments | |
| Combined oral contraceptives (COCs) or “the pill” | Contains two hormones (estrogen and progestogen) | Prevents the release of eggs from the ovaries (ovulation) | >99% with correct and consistent use | Reduces risk of endometrial and ovarian cancer | |
| 92% as commonly used | |||||
| Progestogen-only pills (POPs) or “the minipill” | Contains only progestogen hormone, not estrogen | Thickens cervical mucous to block sperm and egg from meeting and prevents ovulation | 99% with correct and consistent use | Can be used while breastfeeding; must be taken at the same time each day | |
| 90–97% as commonly used | |||||
| Implants | Small, flexible rods or capsules placed under the skin of the upper arm; contains progestogen hormone only | Thickens cervical mucous to block sperm and egg from meeting and prevents ovulation | >99% | Health-care provider must insert and remove; can be used for 3–5 years depending on implant; irregular vaginal bleeding common but not harmful | |
| Progestogen only injectables | Injected into the muscle or under the skin every 2 or 3 months, depending on product | Thickens cervical mucous to block sperm and egg from meeting and prevents ovulation | >99% with correct and consistent use | Delayed return to fertility (about 1–4 months on the average) after use; irregular vaginal bleeding common, but not harmful | |
| 97% as commonly used | |||||
| Monthly injectables or combined injectable contraceptives (CIC) | Injected monthly into the muscle, contains estrogen and progestogen | Prevents the release of eggs from the ovaries (ovulation) | >99% with correct and consistent use | Irregular vaginal bleeding common, but not harmful | |
| 97% as commonly used | |||||
| Combined contraceptive patch and combined contraceptive vaginal ring (CVR) | Continuously releases 2 hormones – a progestin and an estrogen- directly through the skin (patch) or from the ring. | Prevents the release of eggs from the ovaries (ovulation) | The patch and the CVR are new and research on effectiveness is limited. Effectiveness studies report that it may be more effective than the COCs, both as commonly and consistent or correct use. | The Patch and the CVR provide a comparable safety and pharmacokinetic profile to COCs with similar hormone formulations. | |
| Intrauterine device (IUD): copper containing | Small flexible plastic device containing copper sleeves or wire that is inserted into the uterus | Copper component damages sperm and prevents it from meeting the egg | >99% | Longer and heavier periods during first months of use are common but not harmful; can also be used as emergency contraception | |
| Intrauterine device (IUD) levonorgestrel | A T-shaped plastic device inserted into the uterus that steadily releases small amounts of levonorgestrel each day | Thickens cervical mucous to block sperm and egg from meeting | >99% | Decreases amount of blood lost with menstruation over time; Reduces menstrual cramps and symptoms of endometriosis; amenorrhea (no menstrual bleeding) in a group of users | |
| Male condoms | Sheaths or coverings that fit over a man’s erect penis | Forms a barrier to prevent sperm and egg from meeting | 98% with correct and consistent use | Also protects against sexually transmitted infections, including HIV | |
| 85% as commonly used | |||||
| Female condoms | Sheaths, or linings, that fit loosely inside a woman’s vagina, made of thin, transparent, soft plastic film | Forms a barrier to prevent sperm and egg from meeting | 90% with correct and consistent use | Also protects against sexually transmitted infections, including HIV | |
| 79% as commonly used | |||||
| Male sterilization (vasectomy) | Permanent contraception to block or cut the vas deferens tubes that carry sperm from the testicles | Keeps sperm out of ejaculated semen | >99% after 3 months semen evaluation | 3 months delay in taking effect while stored sperm is still present; does not affect male sexual performance; voluntary and informed choice is essential | |
| 97–98% with no semen evaluation | |||||
| Female sterilization (tubal ligation) | Permanent contraception to block or cut the fallopian tubes | Eggs are blocked from meeting sperm | >99% | Voluntary and informed choice is essential | |
| Lactational amenorrhea method (LAM) | Temporary contraception for new mothers whose monthly bleeding has not returned; requires exclusive or full breastfeeding day and night of an infant less than 6 months old | Prevents the release of eggs from the ovaries (ovulation) | 99% with correct and consistent use | A temporary family planning method based on the natural effect of breastfeeding on fertility | |
| 98% as commonly used | |||||
| Emergency contraception pills (ulipristal acetate 30 mg or levonorgestrel 1.5 mg) | Pills taken to prevent pregnancy up to 5 days after unprotected sex | Delays ovulation | If all 100 women used progestin-only emergency contraception, one would likely become pregnant. | Does not disrupt an already existing pregnancy | |
| Standard Days Method or SDM | Women track their fertile periods (usually days 8 to 19 of each 26 to 32 day cycle) using cycle beads or other aids | Prevents pregnancy by avoiding unprotected vaginal sex during most fertile days. | 95% with consistent and correct use. | Can be used to identify fertile days by both women who want to become pregnant and women who want to avoid pregnancy. Correct, consistent use requires partner cooperation. | |
| 88% with common use (Arevalo et al 2002) | |||||
| Basal Body Temperature (BBT) Method | Woman takes her body temperature at the same time each morning before getting out of bed observing for an increase of 0.2 to 0.5 degrees C. | Prevents pregnancy by avoiding unprotected vaginal sex during fertile days | 99% effective with correct and consistent use. | If the BBT has risen and has stayed higher for 3 full days, ovulation has occurred and the fertile period has passed. Sex can resume on the 4th day until her next monthly bleeding. | |
| 75% with typical use of FABM (Trussell, 2009) | |||||
| Two Day Method | Women track their fertile periods by observing presence of cervical mucus (if any type color or consistency) | Prevents pregnancy by avoiding unprotected vaginal sex during most fertile days, | 96% with correct and consistent use. | Difficult to use if a woman has a vaginal infection or another condition that changes cervical mucus. Unprotected coitus may be resumed after 2 consecutive dry days (or without secretions) | |
| 86% with typical or common use. (Arevalo, 2004) | |||||
| Sympto-thermal Method | Women track their fertile periods by observing changes in the cervical mucus (clear texture) , body temperature (slight increase) and consistency of the cervix (softening). | Prevents pregnancy by avoiding unprotected vaginal sex during most fertile | 98% with correct and consistent use. | May have to be used with caution after an abortion, around menarche or menopause, and in conditions which may increase body temperature. | |
| Reported 98% with typical use (Manhart et al, 2013) | |||||
Traditional methods
| Traditional Method | Description | How it works | Effectiveness to prevent pregnancy | Comments | |
| Calendar method or rhythm method | Women monitor their pattern of menstrual cycle over 6 months, subtracts 18 from shortest cycle length (estimated 1st fertile day) and subtracts 11 from longest cycle length (estimated last fertile day) | The couple prevents pregnancy by avoiding unprotected vaginal sex during the 1st and last estimated fertile days, by abstaining or using a condom. | 91% with correct and consistent use. | May need to delay or use with caution when using drugs (such as anxiolytics, antidepressants, NSAIDS, or certain antibiotics) which may affect timing of ovulation. | |
| 75% with common use | |||||
| Withdrawal (coitus interruptus) | Man withdraws his penis from his partner’s vagina, and ejaculates outside the vagina, keeping semen away from her external genitalia | Tries to keep sperm out of the woman’s body, preventing fertilization | 96% with correct and consistent use | One of the least effective methods, because proper timing of withdrawal is often difficult to determine, leading to the risk of ejaculating while inside the vagina. | |
| 73% as commonly used (Trussell, 2009) | |||||
What if I am already pregnant?
Well no need to panic at all, Babies indeed are a blessing. Make sure to take good care of yourself and avoid stress. Reproductive Health Uganda clinics are open and you can visit at any working time, Monday- Saturday or better still, call ahead and set yourself an appointment with our well trained doctors.
Our prices are subsidised and are affordable. RHU boosts of over 60 years experience in providing quality and exceptional reproductive health services.



