Other RHU publications
Category:

The Power to Youth Expedition Magazine
Welcome to a brand-new chapter in 2025! As we reflect on a transformative 2024, with its moments of challenge and triumph, we are thrilled to journey with you once again, each step powered by your passion and ingenuity.
Step into The Power to Youth Expedition, our vibrant hub of empowerment and inspiration.
More than a booklet, this is your creative playground—a space where every story, every achievement, and every vision is a celebration of the change you ignite.
Together, we weave a tapestry of progress, honoring the footprints of yesterday while boldly charting the course for tomorrow.
THE RHU SPOTLIGHT MAGAZINE 2024

Dear Reader,
Greetings from Reproductive Health Uganda!
The year 2024 was nothing short of extraordinary, and we have captured every impactful moment just for you! We are excited to announce the release of the Annual RHU Spotlight Magazine—a captivating collection of stories, insights, and achievements that beautifully showcase our journey throughout the year.
Ready to be inspired?
Dive into a world of thought-provoking discussions, powerful narratives, and creative expressions that push boundaries and spark change. Whether you are a passionate advocate or just beginning to explore this field, there is something special waiting for you in every page.
Flip through the pages, let your curiosity lead the way, and join our community of change-makers.
Your voice matters!
We would love to hear your thoughts! Your feedback helps us grow and continue to bring you content that resonates and inspires.
Are you ready for this adventure?
Explore the Annual RHU Spotlight Magazine now
We’re thrilled to have you as part of our community and can’t wait to hear your insights!
Wishing you an inspiring read.
RHU 2025 WISH LIST
Hello Partners!
Happy New Year 2025!
As we usher in a brand-new chapter filled with promise, possibilities, and purpose, we are brimming with excitement to share our 2025 Wish List with you!
But here’s the kicker: these dreams won’t just remain wishes – they will transform into reality in partnership with YOU – the young changemakers, the generous donors with a heart of gold, and the passionate CSOs driving impact across the globe, the supportive government, the resilient communities we serve and the ever-vigilant fourth estate—the media. Together, we are unstoppable!
So, grab your calendars, dust off your vision boards, and get ready to ignite 2025 with bold ideas, collaboration, and a sprinkle of magic. The best is yet to come!
Let’s do this!

Empowerment Through the Green Jobs Project: Olive Karungi’s Transformation

In the picturesque region of Fort Portal, nestled within the community of Nyankwazi Bwanika, lives Olive Karungi, a widow and mother of three. Olive is a testament to the transformative power of the Green Jobs Project implemented by Reproductive Health Uganda in partnership with WWF. This initiative aims to create and scale green jobs by applying a nature-based solution approach at a landscape level while using Gender Transformative Approach (GTA) as an entry point.
Olive’s journey began when she joined the Kichwamba Youth Vegetable Growers group, a community conservation group supported by Green Jobs project. One of the most profound impacts of the Green Jobs Project has been its role in reducing gender-based violence (GBV) within the community.
“The greatest contributors to GBV are poverty, lack of food, lack of water and making decisions between couples” Olive explains. “Women and girls were often forced to travel long distances to fetch water, exposing them to the risk of sexual exploitation and gender-based violence (SGBV).”
The community groups formed under the project have become safe spaces where members can address GBV issues within families through SRHR community dialogues. These groups have also played a crucial role in demystifying gender roles in the community. Women are now able to make decisions, especially financial ones, which were previously a domain dominated by men.
Through her group, Olive gained essential skills in sustainable agriculture and water management. “We have learned how to grow our own food and effectively store water using tanks built with skills acquired under the project,” Olive shares enthusiastically. This knowledge has been a cornerstone in fostering self-sufficiency and resilience among the community members, particularly in the face of climate-induced adversities.
Olive’s story is one of hope and transformation. The ripple effect of Green Jobs Project has led to improved living standards and enhanced safety for the people of Bwanika.
“This project has brought us together and given us the skills to make our health better. We are now more resilient, more united, and more hopeful for the future,” says Olive.
Through the Green Jobs Project, Reproductive Health Uganda has demonstrated that addressing climate change using GTA can have far-reaching benefits, extending beyond environmental sustainability to encompass social and economic well-being. Olive Karungi’s story, is a powerful reminder of the positive change that can arise when communities are empowered with GTA knowledge and skills to adapt and thrive.

Call for a Consultant to Carry out Operations Research on Sexual and Gender Based Violence in Mbale and Busia Districts, Uganda under the Power to Youth Programme.
Call for a Consultant to Carry out Operations Research on Sexual and Gender Based Violence in Mbale and Busia Districts, Uganda under the Power to Youth Programme.
Terms of Reference for Central Operations Reserach – Power to Youth

The SRHR Spotlight Newsletter
Hello reader,
Welcome back to the SRHR Spotlight Newsletter! Dive into a world of curated insights, thought-provoking discussions, and fresh perspectives with our tales.
Whether you’re a seasoned enthusiast or just starting your journey into our niche, we’ve got something special for you.
Enjoy your reading.
Reproductive Health Uganda

The SRHR Spotlight – October 2023

Uganda Launches the FP2030 commitments
On the 3rd November, Uganda launched the FP2030 commitments. The objective of the launch was to create awareness, understanding and momentum leading to the global launch that is due November 18th 2021. Uganda has made several commitments towards the FP 2030 to address the gaps in ensuring access to family planning commodities.
Reproductive health Uganda alongside other civil society organizations will partner with the Ministry of Health to see the commitments to fruition.
Speaking at the launch, the minister of Health Dr. Jane Ruth Aceng underlined that Government is keen on implementing its commitments on family planning. She said the focus should now change to the boy child.
Speaking at the launch of the Uganda Family Planning 2030 Commitments in Kampala on Wednesday, Aceng said boys ‘need to know the dangers of making a teenage girl pregnant’. ‘The focus has been on the recipient of the pregnancy and not the giver.’
Over the past nine years, governments, civil society, multilateral organizations, donors, the private sector and the research community, have come together around an ambitious goal: to enable 120 million additional women and girls to use modern contraception by 2020. Working together in partnership, much has been achieved, but more remains to be done.
The global family planning community agreed that the gains of the last nine years should be sustained by extending this pivotal partnership. Through a global consultation, stakeholders from around the world provided their input on the future of family planning. Together, the community created a shared vision for 2030 that builds on progress achieved to date, adapts the partnership in response to the lessons of the first nine years and positions us to achieve the future women and girls around the world are asking for.
The collective feedback has formed the basis of a vision, guiding principles, and focus areas. With this foundation, and informed by the family planning community consultation, the new partnership will be built over the course of 2021.
The Uganda Family Planning 2030 Commitments include the following:
– to increase equitable access and voluntary use of modern contraceptive methods for all women and couples
– to increase funding for adolescent sexual and reproductive health programmes
– to ensure contraceptive commodity security
– to strengthen the policy and enabling environment for family planning
– to strengthen the policy and enabling environment for family planning
– to strengthen family planning data use at all levels
– to address family planning myths and misconceptions through evidence-based sexual and behavioral change communication and advocacy
Guiding Principles of the commitments
- Voluntary, person-centered, rights-based approaches, with equity at the core: This guiding principle reflects the fundamental belief that individuals should be able to freely make choices that reflect their desires and needs. Every decision, action, and investment made by the partnership will reflect this belief – that each person has the same right to quality family planning, regardless of their geography, socioeconomic status, gender, or culture.
- Empowering women and girls and engaging men, boys, and communities: Positive male inclusion is needed to truly transform normalization of family planning and at the same time share the burden of the decisions and implications of family planning. This must happen in tandem with empowerment of women and girls to create true equity.
- Building intentional and equitable partnerships with adolescents, youth, and marginalized populations to meet their needs, including for accurate and disaggregated data collection and use: These populations have been consistently underserved, so the partnership commits to prioritizing them in all future work.
- Country-led global partnerships, with shared learning and mutual accountability for commitments and results: Country commitments drive progress with support from regional and global stakeholders for implementation, coordination, and accountability.

Tips for working from home successfully
Following the outbreak of the Novel Corona virus world wide, most of us have been forced to work from home. We have come up with a few tips to help you work efficiently and effectively from home. Click here to learn more RHU-ICT-COVID-19 WFH

Not ready to get pregnant yet? Here are a few things you could do
These are very unprecedented times. We are no longer dealing with the same challenges as we were before. Times where we knew how not to spread HIV/AIDS or at least contain it. We could easily treat or prevent Sexually Transmitted Infections and disease (STDs/STIs). And now? Chlamydia, Gonorrhoea, Syphilis and even THE HIV/AIDs itself are no match for the Novel Corona virus.
These are indeed very uncertain times, with governments all over the world taking drastic measures to lock down, restrict movements and yet with diminutive hope or certainty that things will go back to normal soon.
Take caution :
With most people working from home or on forced leave and movement restrictions, loneliness, boredom with the so much time is paramount. For those staying with their partners the idea of sex must be flaunting. I mean ‘things’ are freely available on full time basis right?
Please note: Even if you are under self or institutional quarantine, having unprotected sex will still expose you to STIs and STDs and unplanned pregnancies.
But since abstinence is a complicated subject even without the CORONA virus, how can one enjoy their things without fear of getting pregnant or contracting STDS or STIs?
How do i not get pregnant?
Using contraceptives allows people to attain their desired number of children and determine the spacing of pregnancies. They are also very helpful in times such as these where one wouldn’t want to get pregnant.
There are however two methods one can use to delay pregnancy; Traditional and modern methods these are broken down below;
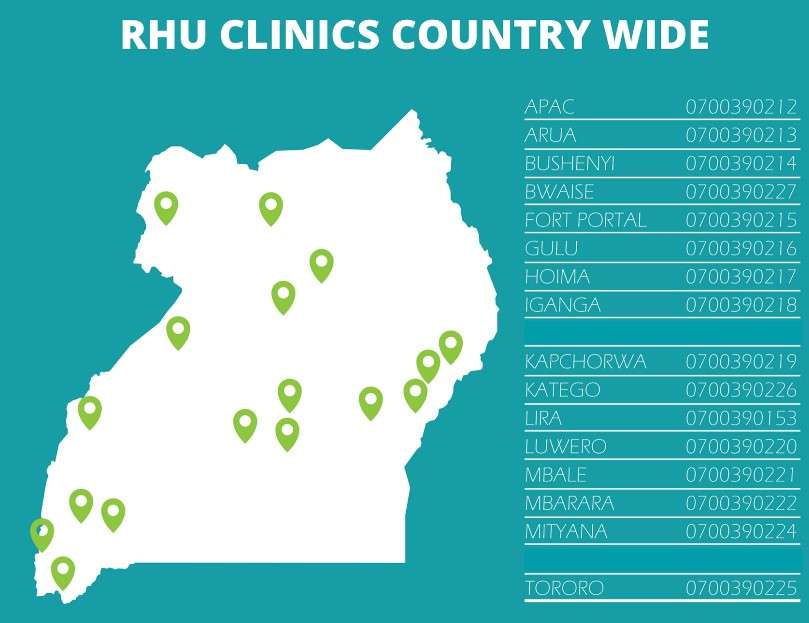
Reproductive Health Uganda clinics remain open across the country You can call any of the clinics in charges for appointments and or questions
What are the Modern methods?
PS: We recommend using modern methods because of their accuracy. They can easily be relied on without fear. These methods are available at any of the Reproductive Health Clinics countrywide. Give us a call to make an appointment
| Method | Description | How it works | Effectiveness to prevent pregnancy | Comments | |
| Combined oral contraceptives (COCs) or “the pill” | Contains two hormones (estrogen and progestogen) | Prevents the release of eggs from the ovaries (ovulation) | >99% with correct and consistent use | Reduces risk of endometrial and ovarian cancer | |
| 92% as commonly used | |||||
| Progestogen-only pills (POPs) or “the minipill” | Contains only progestogen hormone, not estrogen | Thickens cervical mucous to block sperm and egg from meeting and prevents ovulation | 99% with correct and consistent use | Can be used while breastfeeding; must be taken at the same time each day | |
| 90–97% as commonly used | |||||
| Implants | Small, flexible rods or capsules placed under the skin of the upper arm; contains progestogen hormone only | Thickens cervical mucous to block sperm and egg from meeting and prevents ovulation | >99% | Health-care provider must insert and remove; can be used for 3–5 years depending on implant; irregular vaginal bleeding common but not harmful | |
| Progestogen only injectables | Injected into the muscle or under the skin every 2 or 3 months, depending on product | Thickens cervical mucous to block sperm and egg from meeting and prevents ovulation | >99% with correct and consistent use | Delayed return to fertility (about 1–4 months on the average) after use; irregular vaginal bleeding common, but not harmful | |
| 97% as commonly used | |||||
| Monthly injectables or combined injectable contraceptives (CIC) | Injected monthly into the muscle, contains estrogen and progestogen | Prevents the release of eggs from the ovaries (ovulation) | >99% with correct and consistent use | Irregular vaginal bleeding common, but not harmful | |
| 97% as commonly used | |||||
| Combined contraceptive patch and combined contraceptive vaginal ring (CVR) | Continuously releases 2 hormones – a progestin and an estrogen- directly through the skin (patch) or from the ring. | Prevents the release of eggs from the ovaries (ovulation) | The patch and the CVR are new and research on effectiveness is limited. Effectiveness studies report that it may be more effective than the COCs, both as commonly and consistent or correct use. | The Patch and the CVR provide a comparable safety and pharmacokinetic profile to COCs with similar hormone formulations. | |
| Intrauterine device (IUD): copper containing | Small flexible plastic device containing copper sleeves or wire that is inserted into the uterus | Copper component damages sperm and prevents it from meeting the egg | >99% | Longer and heavier periods during first months of use are common but not harmful; can also be used as emergency contraception | |
| Intrauterine device (IUD) levonorgestrel | A T-shaped plastic device inserted into the uterus that steadily releases small amounts of levonorgestrel each day | Thickens cervical mucous to block sperm and egg from meeting | >99% | Decreases amount of blood lost with menstruation over time; Reduces menstrual cramps and symptoms of endometriosis; amenorrhea (no menstrual bleeding) in a group of users | |
| Male condoms | Sheaths or coverings that fit over a man’s erect penis | Forms a barrier to prevent sperm and egg from meeting | 98% with correct and consistent use | Also protects against sexually transmitted infections, including HIV | |
| 85% as commonly used | |||||
| Female condoms | Sheaths, or linings, that fit loosely inside a woman’s vagina, made of thin, transparent, soft plastic film | Forms a barrier to prevent sperm and egg from meeting | 90% with correct and consistent use | Also protects against sexually transmitted infections, including HIV | |
| 79% as commonly used | |||||
| Male sterilization (vasectomy) | Permanent contraception to block or cut the vas deferens tubes that carry sperm from the testicles | Keeps sperm out of ejaculated semen | >99% after 3 months semen evaluation | 3 months delay in taking effect while stored sperm is still present; does not affect male sexual performance; voluntary and informed choice is essential | |
| 97–98% with no semen evaluation | |||||
| Female sterilization (tubal ligation) | Permanent contraception to block or cut the fallopian tubes | Eggs are blocked from meeting sperm | >99% | Voluntary and informed choice is essential | |
| Lactational amenorrhea method (LAM) | Temporary contraception for new mothers whose monthly bleeding has not returned; requires exclusive or full breastfeeding day and night of an infant less than 6 months old | Prevents the release of eggs from the ovaries (ovulation) | 99% with correct and consistent use | A temporary family planning method based on the natural effect of breastfeeding on fertility | |
| 98% as commonly used | |||||
| Emergency contraception pills (ulipristal acetate 30 mg or levonorgestrel 1.5 mg) | Pills taken to prevent pregnancy up to 5 days after unprotected sex | Delays ovulation | If all 100 women used progestin-only emergency contraception, one would likely become pregnant. | Does not disrupt an already existing pregnancy | |
| Standard Days Method or SDM | Women track their fertile periods (usually days 8 to 19 of each 26 to 32 day cycle) using cycle beads or other aids | Prevents pregnancy by avoiding unprotected vaginal sex during most fertile days. | 95% with consistent and correct use. | Can be used to identify fertile days by both women who want to become pregnant and women who want to avoid pregnancy. Correct, consistent use requires partner cooperation. | |
| 88% with common use (Arevalo et al 2002) | |||||
| Basal Body Temperature (BBT) Method | Woman takes her body temperature at the same time each morning before getting out of bed observing for an increase of 0.2 to 0.5 degrees C. | Prevents pregnancy by avoiding unprotected vaginal sex during fertile days | 99% effective with correct and consistent use. | If the BBT has risen and has stayed higher for 3 full days, ovulation has occurred and the fertile period has passed. Sex can resume on the 4th day until her next monthly bleeding. | |
| 75% with typical use of FABM (Trussell, 2009) | |||||
| Two Day Method | Women track their fertile periods by observing presence of cervical mucus (if any type color or consistency) | Prevents pregnancy by avoiding unprotected vaginal sex during most fertile days, | 96% with correct and consistent use. | Difficult to use if a woman has a vaginal infection or another condition that changes cervical mucus. Unprotected coitus may be resumed after 2 consecutive dry days (or without secretions) | |
| 86% with typical or common use. (Arevalo, 2004) | |||||
| Sympto-thermal Method | Women track their fertile periods by observing changes in the cervical mucus (clear texture) , body temperature (slight increase) and consistency of the cervix (softening). | Prevents pregnancy by avoiding unprotected vaginal sex during most fertile | 98% with correct and consistent use. | May have to be used with caution after an abortion, around menarche or menopause, and in conditions which may increase body temperature. | |
| Reported 98% with typical use (Manhart et al, 2013) | |||||
Traditional methods
| Traditional Method | Description | How it works | Effectiveness to prevent pregnancy | Comments | |
| Calendar method or rhythm method | Women monitor their pattern of menstrual cycle over 6 months, subtracts 18 from shortest cycle length (estimated 1st fertile day) and subtracts 11 from longest cycle length (estimated last fertile day) | The couple prevents pregnancy by avoiding unprotected vaginal sex during the 1st and last estimated fertile days, by abstaining or using a condom. | 91% with correct and consistent use. | May need to delay or use with caution when using drugs (such as anxiolytics, antidepressants, NSAIDS, or certain antibiotics) which may affect timing of ovulation. | |
| 75% with common use | |||||
| Withdrawal (coitus interruptus) | Man withdraws his penis from his partner’s vagina, and ejaculates outside the vagina, keeping semen away from her external genitalia | Tries to keep sperm out of the woman’s body, preventing fertilization | 96% with correct and consistent use | One of the least effective methods, because proper timing of withdrawal is often difficult to determine, leading to the risk of ejaculating while inside the vagina. | |
| 73% as commonly used (Trussell, 2009) | |||||
What if I am already pregnant?
Well no need to panic at all, Babies indeed are a blessing. Make sure to take good care of yourself and avoid stress. Reproductive Health Uganda clinics are open and you can visit at any working time, Monday- Saturday or better still, call ahead and set yourself an appointment with our well trained doctors.
Our prices are subsidised and are affordable. RHU boosts of over 60 years experience in providing quality and exceptional reproductive health services.
